Takeaway
Writing or drawing after a challenging patient encounter may help you work through your feelings and mitigate burnout.

Passion in the medical profession | February 1, 2021 | 4 min read
By Megan Gerber, MD, MPH, Albany Medical College
Listening is integral to giving clinically excellent patient care. As physicians, we bear witness to accounts of injury, suffering, and loss, juxtaposed with narratives of recovery, healing, and joy. After years of working with trauma-exposed women, I went through a period in which things were “getting to me.” I felt angry on behalf of my patients, frustrated with care processes and colleagues, and periodically found myself tearful after work. When vivid dreams started, I realized I might be experiencing vicarious traumatization which occurs when clinicians experience negative transformative processes, a change in inner experience or system of meaning as a result of engagement over time with trauma survivors. This was never talked about in my training. Instead, we were expected to steel ourselves against human stories and not “allow them in.”
I was aware of what experiencing trauma did to my patients’ bodies and minds, but did I understand the impact it had on me? As a medical educator, could I mentor learners if I didn’t understand this myself? Listening to accounts of injury, pain, and societal injustice can be countered by the privilege and joy of accompanying our patients on their often slow, sometimes tortuous journey toward healing. After blunt physical injury, tissues heal more-or-less predictably in a complex and elegant cascade of bleeding, clotting and granulation that brings changes in color, texture, and sensation. Mind and spirit also recover from trauma, but in a manner less linear, exact, and certain. This process is highly individual and involves an intricate interplay between one’s own epigenetics, life experiences, temperament, and access to resources. Each person brings unique strengths and vulnerabilities to this healing trajectory which is less of a well-delineated pathway and more fluid and freeform.

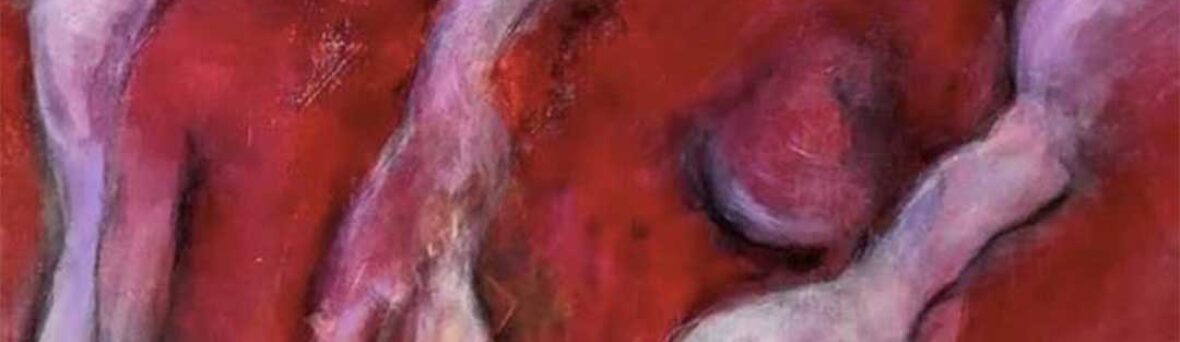
I painted my abstract acrylic, “Granulation,” after a challenging week in clinic. I believe it depicts the relationship between the more precise pathways of tissue repair and the idiosyncratic process of healing mind and spirit. Rather than trying to depict a discrete object or scene, I allowed myself to just feel and paint. The background of the painting was created using multiple thin layers of paint applied with a dry brush and rags that evoke depth and the raw granular texture of cells and tissues. I applied and removed paint until I achieved this variegated effect. Superimposed on this are soft, weightless, humanoid forms that arise from the background and appear to float above it, untethered, representing the unscripted aspects of healing mind and spirit. The lightness of these forms suggests that healing from trauma, although challenging, can be a liberating and sometimes joyful experience if we allow ourselves to appreciate and see it. The painting’s dominant color, red, represents not only blood and viscera but passion and energy. I created a series of abstractions, and in doing so found myself feeling less frustrated and helpless in clinic. My troubling dreams eventually stopped.
Abstract art departs from exactitude and enables us to freely communicate visually without the constraints of forms found in objective reality. Here, it enabled depiction of the difficult to describe aspects of recovery and reduced my own distress. Painting has become my way of releasing the pain of others from my own cells and capturing the inexact trajectory and beauty of recovery from trauma and injustice.
Research has demonstrated that mindfulness-based art therapy reduces anxiety, perceived stress, and salivary cortisol levels. Thus, perhaps making art can play a bigger role in professional sustainment and mitigating burnout. Braus and Morton recently suggested that the proliferation of creative projects during the COVID-19 pandemic is a form of art therapy that lessens the negative mental health impact of isolation. Recently, in addition to discussing our reactions to patients’ histories, I’ve offered my students the opportunity to write or draw after difficult encounters when time permits.
An important component of trauma-informed care is recognizing the impact working with patients has on us and searching for our own definitions of healing. This is an important lesson we must learn and impart. I would never have thought that painting would make me a better and more resilient listener for my patients, but it has.
5 tips for creating visual art to process challenging clinical encounters:
1. Choose a simple medium like colored pencils, oil pastels, or watercolors.
2. If you find painting or drawing daunting, try collaging with magazine/catalog images or tissue paper.
3. Give yourself permission not to care about the final product. Focus on the process. Remind yourself there’s no need to consciously depict anything.
4. If mindfulness or breathing exercises are helpful to you, engage in this before starting your piece artwork. Listening to music is helpful for some.
5. Visualize what you’re feeling. If the feeling were an object what color, weight, and texture would it have?

This piece expresses the views solely of the author. It does not represent the views of any organization, including Johns Hopkins Medicine.